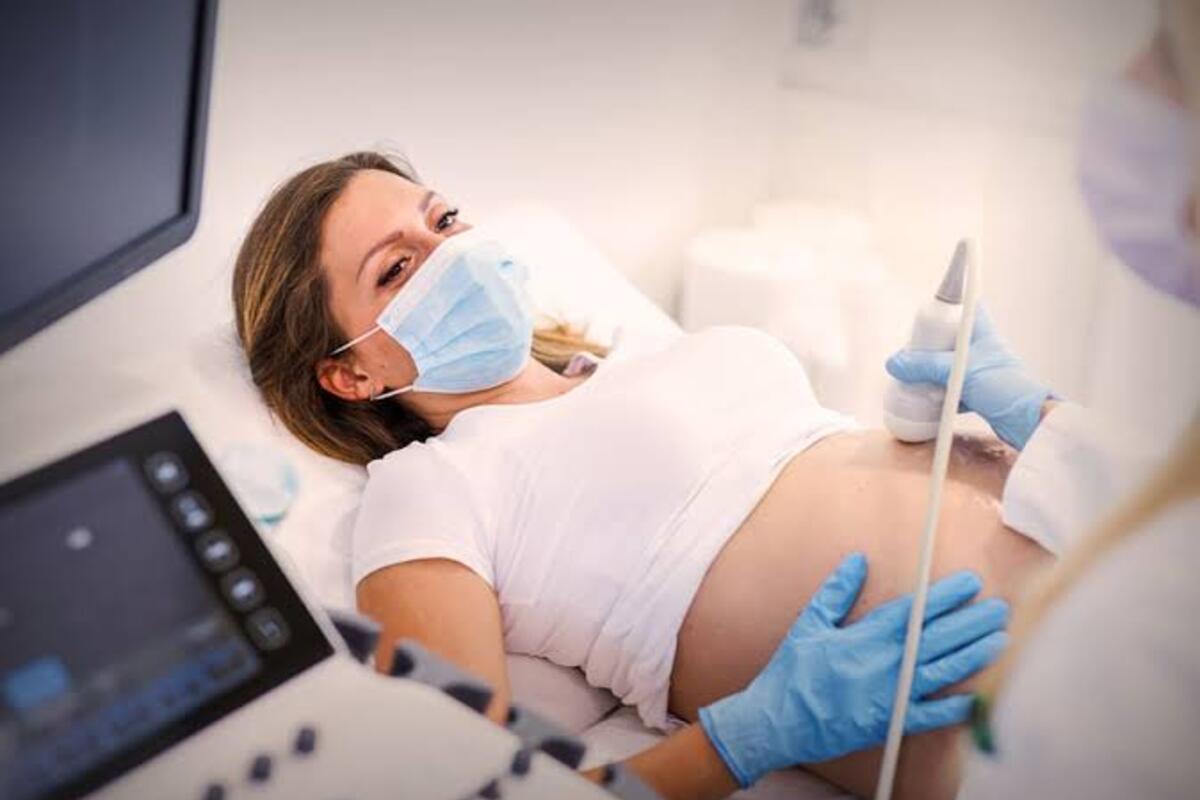
A recent analysis of nearly 2.8 million pregnancies between 2016 and 2022 found that stillbirths in the United States are more common than previously reported, with a significant number of them striking without warning.
The study published on Monday and led by researchers at Harvard and Mass General Brigham, revealed that about 30% of stillbirths occur in pregnancies that did not appear linked to any previously identified health or clinical risks. The study also found that stillbirth continues to fall unevenly along racial and socioeconomic lines, with Black families and poorer communities being hit hardest.
In a statement made by Mark Clapp, an obstetrician and maternal-fetal medicine specialist at Massachusetts General Hospital and one of the study authors, he stated that better screening and monitoring are urgently needed as a result of this new discovery. He also explained that every stillbirth represents an unimaginable loss, not just for the mother but for the entire family, and is a reminder of how far we still have to go.
Between 2016 and 2022, the study found stillbirth rates of approximately 1 in 95 births in areas with a higher proportion of Black families, 1 in 112 for low-income families, and 1 in 147 overall, which is higher than the CDC’s reported rate of 1 in 175.
According to Jessica Cohen, co-senior author and professor of health economics at the Harvard T.H. Chan School of Public Health, she stated that the discrepancy in rates between the study and CDC data could be due to known inaccuracies in the recording of fetal death certificates, which don’t always accurately capture every stillbirth and varies in quality and definition across states.
Stillbirth is defined as the death of a fetus after 20 weeks of pregnancy. It has seen its decline slow despite overall downward trends over the past 30 years. While more than 70% of stillbirths are linked to risk factors like obesity, substance use, or diabetes, the study revealed that many still occur without a known cause. Specific risk factors include chronic hypertension, fetal anomalies, low amniotic fluid, and post-41 weeks of gestation, which significantly increases the risk.
The study also revealed that structural inequities, including where a person lives and the resources available in their community are strong predictors of stillbirth risk. Meanwhile, higher rates were found in low-income and predominantly Black areas, even for those with private insurance.
The authors suggested that social disadvantage continues to determine pregnancy that stem beyond simple access to care. They further added that even in cities with high-quality hospitals, some women tend to be afraid to advocate for themselves or question medical decisions.